Factory health care service between 19501988
Already in the 1800s the workers in Hungary established aid associations
to get support in case of sickness or disability. In 1970 the first General
Aid Fund for Sick and Disabled Workers was established, which provided
free medical care, medication and financial aid for its members. Todays
factory health care can be traced back to the doctors working for the aid
associations and the sickness-insurance of workers. Later, the treatment
of workers became more organised within the framework of the National Workers
Insurance Fund and then the National Social Insurance Institute (OTI).
Recognising the importance of occupational diseases
OTI established a Lead Control Station in 1934 and periodic examination
of the exposed workers became a rule. In 1940 the task of the Station was
expanded and it was developed into an Occupational Disease Examining Station
with adequate laboratory background (Kapronczay 1988, Ungváry 1994).
Between World Wars I and II many factories (both
those owned by the state and private ones) employed factory physicians,
whose responsibility was the performance of fitness-for-work examinations
and the treatment of the sick workers.
Hospitals were also built near the biggest factories
by the owners for the treatment of the workers and sometimes also their
family members (Csepel, Diósgyõr, Pécsbányatelep).
After World War II, provision of health care for
workers became pressing, because in 194546 a survey initiated by the Ministry
of Industry in 1923 factories, proved that the health of the undernourished
workers was gravely endangered due to extremely unhealthy working conditions.
This survey also proved that the working environment
was much more dangerous than any other part of the environment, for example
the dwelling environment. The decisive role of this circumstance became
obviously one of the main reasons of the poor state of health of the workers.
Due to the unfavourable working conditions, a great number of the so called
classic occupational diseases appeared in grave form, following a short
latency period (Ungváry 1993).
After 1945, on the initiative of the trade unions,
the training of occupational physicians began and their number quickly
increased (150 physicians participated in the first training course). At
that time (similarly to the pre-war period) physicians and nurses were
employed by the factories, there was no demand for harmonised professional
guidance, moreover it was not possible at all.
In 1951 a state-organised factory health care service
was established. An organisational, operational code was published in the
same year, which identified the tasks. It is worth to review this, because
the basic ideas remained the same for the following decades. (Ungváry
1993).
The main responsibilities of the factory physicians were:
1. Curative-preventive care. This task involved:
pre-employment and periodic medical examination of the workers and
examination when changing their job;
treatment of the workers;
participation in deciding to put diseased workers on the sick-list
and in the supervision of those on sick allowance;
statistical analysis of the diseases of factory workers;
recording and reporting of work-accidents, occupational diseases,
poisonings, infectious diseases;
study and identification of the causes the probable work-related
diseases;
organisation of care for factory workers with the aid of care institutions
and other health institutions (hospitals, polyclinics), regarding
pregnant and lactating women;
adolescents;
old people;
workers with limited working ability;
disabled;
those who were regularly or frequently ill;
workers with TBC;
workers with venereal disease;
workers with gastric or duodenal ulcer;
workers with organic heart disease and hypertension;
diabetics;
workers with cancer;
workers with trachoma;
those working in jobs under extremely hazardous conditions.
At that time factory physicians were not responsible to judge the workers fitness for work (they were entitled to give one day sick leave, or three days during the epidemics of contagious upper airway diseases). They treated mainly acute cases and cared for workers with chronic diseases, who were able to work.
2. Public health activity. These tasks included:
inspection of health conditions of the factory at least bi-annually,
involving the occupational nurse, keeping the records of factory visits;
participation at the monthly inspection by the management;
preparation of plans for the development of occupational health in
the factory;
supervision of the building plans of the factory with the involvement
of the factory safety officer;
setting health standards prior to the introduction of methods hazardous
to health and to use of new materials with health hazards, together with
the safety officer;
participation in the planning of investment, development, and refurbishment
in connection with factory health of the factory;
regular inspection of the factory kitchen, canteen and catering with
the help of the factory nurse;
regular public health inspection of the welfare institution and training
workshop of the factory.
Unfortunately, due to many reasons, these tasks were more and more
neglected.
3. First aid activity. To this belonged:
organisation of first aid in the factory, guidance and control of
the work of the first aid stations and first aid training, control of the
quality and quantity of medicines and dressings used for first aid.
4. Activity regarding the factory health protection regulation
This activity stopped when the protection regulations were cancelled.
5. Other tasks. To this belonged:
maintaining of close contact with the Red Cross and co-operation
with it, within the factory;
recommendation for providing protective ointments and protective
food;
suggestion for the assignment to suitable jobs of pregnant, lactating
women and workers who suffered occupational diseases.
The heads of the local Health Departments had the
right to employ factory physicians whose salaries had to be covered by
the budget of the local councils. Disciplinary matters involving physicians
were also handled by Health Department heads. Health Departments were entitled
to join factory physician consulting rooms to the respective territorial
polyclinic. The head of the territorial polyclinic was responsible for
the material supply of the factory physician consulting room;
organising monthly workshops for the factory physicians at the polyclinic;
the regular control of their work and discipline;
their professional training.
Professional guidance of the occupational health
network was the responsibility of the county, town chief physicians, based
on the views published by the Ministry of Health. The professional activity
of the newly organised National Institute for Occupational Health made
its way indirectly through the Ministry of Health.
In 1951 the State Sanitary and Epidemiological Inspectorate
was organised. The state sanitary inspectors worked within the organisation
of the council health departments, to control the observance of public
health norms regulated by law and other orders related to public health
issues in their areas of activity such as industrial, transport and catering
firms. The connection between the factory health care service and the public
health inspectorates was realised through the council health departments.
In 1954 State Sanitary and Epidemiological Stations
were established, with occupational health departments in their county
institutes, led by physicians specialised in sanitary-epidemiology and
experienced in occupational hygiene. Laboratories in the county institutes
became increasingly capable of performing instrumental examinations of
the workplace factors. The factory health service and occupational hygienists
were connected in the fields of both service and authority work (Ungváry
1993).
From the late 1950s there was a growing demand for
the curative and related preventive activities of factory physicians. This
activity in the factory physicians office was necessary mainly due to
the growing number of workers who went to work in the factory daily from
the neighbouring villages. At that time the increase of production was
ensured by the increase of the staff. At the same time the coverage by
general practitioners was unsatisfactory, particularly at the small places.
One physician had to provide care for the population of several villages
and the workers coming home from work were unable to meet the home physician
during the consultation hours. Beginning from 1961, this activity involved
also the judgement of fitness for work, first in the biggest factories,
later also in most of the medium-sized factories.
The legislative regulation on occupational rehabilitation
came into effect in 1967, though such caritative activity had occurred
earlier mainly in the big factories. The precondition of successful occupational
rehabilitation makes both employers and employees interested. Though the
basic order was several times amended, no solution was provided for promotion
of interest; so the problem of occupational rehabilitation remained unsolved,
particularly in those cases, when it was impossible to rehabilitate someone
at his/her original workplace.
In the field of factory health care a significant
milestone was the new possibility of obtaining the occupational health
specialist degree in 1968. The Department of Occupational Hygiene
and Medicine of the Postgraduate Medical School was established and with
contribution of the staff of the National Institute for Occupational Health,
it became the guiding centre of postgraduate education.
Terms of reference of factory health care were formulated
by the Health Act in 1972, a summary of the previous regulations. According
to this, the responsibility of factory health care is the provision
of treatment and prevention for workers at the workplace and the promotion
of the enforcement the work-related public health requirements. Promotion
of the enforcement the work-related public health requirements meant that
factory health care had no authority rights and could not enforce the public
health requirements.
Several regulations were attached to the Health
Act, e.g. a ministerial order regulated the provision of treatment and
prevention for workers at the workplace, including the guiding number of
staff according to branches.
According to the above mentioned regulations a factory
health care service had to be organised and maintained in every
mine, foundry, chemical, food industrial plant and construction site,
where at least 300;
iron works, where at least 400;
other plants and factories, furthermore agricultural co-operatives,
state farms, where at least 500 workers were employed.
In addition, a full-time factory physician had to
be employed in the firms belonging to the first group above for every 1200,
belonging to the second group above for every 1400, and belonging to the
third group above for every 16001800 worker, respectively. In the biggest
firms factory health consultancies (surgery, gynaecology, laboratory, dermatology,
etc.) were organised.
This order regulated also the financial side of
the establishment and maintenance of factory health care service. According
to this, furnishing and equipment of medical nature and all material expenses
had to be covered by the maintaining council from its budget. The provision
of the premises required to establish factory health care service together
with its maintenance were the responsibility of the employer.
This enacting close summarised the tasks of the
service as well as the responsibilities of the head of the service and
those of the head of the firm. Separate articles referred to the topic
of first aid at the workplace.
At this time two levels developed for the treatment
of occupational diseases, the first was the factory health care service
in the factories, the second was the care provided by the occupational
health consultations and the in-patient department of the National Institute
for Occupational Health.
In 1975 there was a significant change of the professional
guidance and organisation of the factory health care network. From this
time on, professional guidance and control were carried out directly by
the National Institute for Occupational Health, with the contribution of
the inspecting chief factory physicians. The Factory Polyclinic of the
Csepel Iron Works (the biggest institution in Hungary of this kind) turned
into a basis for organisation and methodology of the national institute
and was incorporated into it (Fig. 1).
Due to the organisational changes of the factory
health care, the services became parts of the health institutions, and
were guided locally by the occupational health deputy directors. This was
the beginning of the organisation of factory health consultations that
handled occupational out-patients on a higher level, and at the same time,
provided factory health care for the employees of the small enterprises.
This way three levels had been developed for the coverage of occupational
health outpatients. These were:
primary care;
factory health consultations;
consultations and in-patient departments of the National Institute.
Noteworthy is the fact that one internal department
of the Central hospital in each county was appointed, where along with
the other patients patients with occupational diseases could be referred
for hospital treatment. In practice, however, this type of provision never
worked because of lack of demand.
In 1979 a new regulation for organisation and
operation of the factory health care service was issued, covering the
whole range of its tasks (Ungváry 1993). In order to take into account
the special characteristics of the different industrial branches the organisation
of the Occupational Health Bases was begun on the fields of mining, textile
industry, road-traffic, oil industry, foundry and metallurgy as well as
agriculture. This theoretically good idea was made inefficient by the rule
that the field of activity of the Bases was limited to the very county
where their headquarters were founded.
At the beginning of the 1980s (between 1981 and
1983) the orders governing the work of factory physicians were amended.
The factory health care service became fully developed in the industrial
branches and in the bigger farms and agricultural co-operatives. In the
year 1989, 2989 factory physicians and 500 factory-district physicians
were employed in the fully developed factory health care service.
During its stay the factory health care service
tried to comply with the demands appearing in different periods of economic
development and arising from the national health (within this mainly medical)
coverage and from the widening of social security service. The factory
health care service deserves to be credited, because due to its activity
a great number of grave occupational diseases occurring after the war disappeared
or after a longer latency period only few and mild cases occurred (Fig.
2). The service did its best to prevent occupational diseases,
by periodic fitness-for-work medical examinations. It deserves mentioning
that the reporting and investigation of overexposure cases were made compulsory
in Hungary which was among the first countries to have a regulation of
this kind in the world. This resulted in a significant decrease of the
incidence of occupational poisonings.
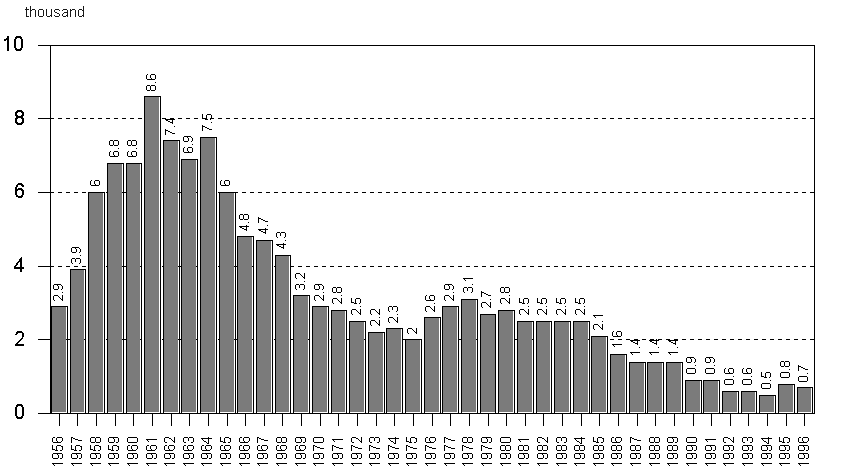
Figure 2. Reported occupational diseases and poisonings (altogether)
Activities of the factory health care service included
health
information and education on the right behaviour at the workplace and
on a healthy life style. It is very difficult to evaluate the effectivity
of this activity as it is not known what the morbidity and mortality indices
of the working population without this activity were. Knowing the present
data on these indices, one can assume that health information and education
activities have not reached the expected results.
Besides the unquestionable results, a number of
mistakes delayed the continuous updating of the service. Among these the
prevalence of curative activity should be mentioned first, which was about
judging the fitness for work. This was not justified already in the 80s,
moreover, it became a drawback by surpassing the preventive activity (Ungváry
1993).
Factory health care consultation and the small enterprises
Factory health care could not cope with the provision for small enterprises,
though the demand for this was only moderate (the majority of small, medium
and big enterprises had their own factory health service). Except of fitness
for work examinations for the small enterprises, factory health consultation
performed hardly any other activity. Since the second part of the 70s,
factory
health care has belonged definitely to the organisations
providing primary health care. Together with this or because of this,
there was generally no lasting and operative connection between factory
physicians and general practitioners, despite the fact that outpatient
workers were generally provided for by factory physicians and bed-patients
were always treated by general practitioners. Their relationship was often
characterised by some kind of rivalry. The smallest villages were exceptions
where the factory physician and the general practitioner was the same person
(so called factory-district physician). The co-operation was hindered also
by the lack of appropriate regulation. All this resulted in many overlappings,
parallelity, duplications and at the same time a considerable part of the
workers (4048%) was deprived of satisfactory health care.
In summary, factory health care service, together
with its results and mistakes, achieved a high standard and practically
prepared the way for the transition into occupational health service, which
was difficult and full of conflicts.
Factory health care provided for about 1,4 million and 1,1 million employees
in 1991 and 1993, respectively. In 1992 the minister of welfare dissolved
the factory health care services. In 1993 the number of factory physicians
was half of that in 1989 (Table 1).
| Service | Specialist consultation | Factory-district
physicians |
|||||
| Year | Full-time | Part-time | All | Full-time | Part-time | All | |
| 1990 | 899 | 1404 | 2303 | 80 | 94 | 174 | 498 |
| 1991 | 853 | 1326 | 2179 | 89 | 154 | 243 | 203 |
| 1992 | 654 | 1178 | 1832 | 87 | 141 | 228 | cancelled |
| 1993 | 551 | 1047 | 1598 | 88 | 138 | 226 | |
| 1994 | 520 | 935 | 1455 | 97 | 151 | 248 | |
| in 1989 | 127 |
| in 1990 | 136 |
| in 1991 | 146 |
| in 1992 | 125 |
| in 1993 | 141 |
| in 1994 | 248 |
The number of physicians (full-time and part-time together) providing
factory health consultation was:
| in 1989 | 178 |
| in 1990 | 174 |
| in 1991 | 243 |
| in 1992 | 228 |
| in 1993 | 226 |
| in 1994 | 248 |
Factory health consultations were provided for about
800 employees per year between 1991 and 1993. This provision, however,
did not include any factory hygiene or preventive hygienic activity.
For the years 1991 and 1993 the distribution of
physicians carrying out factory health consultation according to specialisation
is the following: in 1991 20% occupational health specialists, 64% other
specialists, 16% non-specialised physicians. In 1993 40% occupational health
specialists, 56% other specialists, 4% non-specialised physicians. There
are fewer occupational health specialists among those taking part in factory
health consultations than among those working in the factory consulting
rooms.
In 1991 there were 244 qualified assistants at the
factory wards, in 1993 the number was 252.
| Year | Fitness for job
examinations |
First-aid | Ongoing care | Other treatment | Total |
| 1989 | 2271 | 307 | 1324 | 6567 | 10471 |
| 1990 | 1973 | 290 | 1245 | 5882 | 9381 |
| 1991 | 1576 | 220 | 1059 | 5066 | 7922 |
| 1992 | 1236 | 168 | 0738 | 3820 | 5961 |
| 1993 | 0982 | 129 | 0556 | 2736 | 4405 |
| 1994 | 1409 | 118 | 0546 | 2589 | 4008 |
| in 1989 | 772 203 |
| in 1990 | 722 476 |
| in 1991 | 863 951 |
| in 1992 | 748 895 |
| in 1993 | 588 691 |
| in 1994 | 554 633 |
In contrast to the expectations, this work is not
increasing either. An increase was expected because the task of factory
health care consultation is to provide for small enterprises, the number
of which significantly increased already in the early 90s. The reason for
this may be the loose control and lack of specific knowledge of the new
entrepreneurs.
Besides the above mentioned tasks, the county and
large town factory health consultations also give advice in the diagnosis
of occupational diseases. Another opinion on job-fitness is given here
too. This consultative service usually working within health institutions
utilises the diagnostic and advisory possibilities provided by the institutions
(laboratory, X-ray, specialists, etc.). Supervision of workplaces is not
within the terms of reference of the factory health care consultative service.
By 1995 a total organisational and operational
crisis of the factory health care service developed: it became obvious
that the state factory health care service adapted to the large enterprises
is unable to provide for the small, mainly privately owned enterprises.
Considering these, the aim of the occupational
health service is the provision of the optimal or near optimal workplace
stress of the workers. For this purpose the service determines and continuously
monitors the individuals ability to cope with stress and the matching
optimal physical, physiological, psychic strain, and it monitors and helps
by advising to keep the workplaces pathogenic (physical, chemical, biological,
psychosomatic, ergonomic) factors at an acceptable level. The new occupational
health service, which should cover all employees, is expected to meet the
professional and structural requirements and at the same time to join functionally
the new Hungarian health care system with insurance-based funding, modified
by the basic reform processes. The occupational health care should cover
all employees, at all firms, in all economic areas (ILO Convention 161,
article 3).
As it was demonstrated earlier, the Hungarian
factory health care adapted to state owned big enterprise economy was not
able to cope with this task. One reason of this was the significant
number of not satisfactorily specialised physicians working in the service.
The physicians not specialised in occupational health had not even theoretical
knowledge on workplace prevention. The other reason and maybe the more
determinant was that the Hungarian regulation expected therapeutic activity
from physicians of the service first. These together caused that the Hungarian
factory health care was unable to meet the challenges arising from professional
development, and to cope with the preventive and health promotion tasks,
got
into professional crisis, its attitude and activity were lagging behind
modern expectations. In 1995 the need for a change became urgent, because
of the signs of crisis and being below the standard in professional development.
The organisational, functional and financial principles
of the essence of the transformation were worked out by the National Institute
of Occupational Health and the Department of Occupational Hygiene and Medicine
of the Postgraduate Medical School jointly with the Scientific Society
of the Hungarian Factory Physicians and the Factory Physicians Section
of the Hungarian Medical Chamber. In 1991 the first conception on the professional,
organisational, and financial transformation of the service was submitted
to the Ministry of Welfare by the four leaders of the above mentioned institutions.
The idea was accepted by the ministry, but no progress was made despite
the fact that the Labour Protection Act (XCIII/1993) came into effect on
1 January 1994. This Act declares that in Hungary every employee has the
right to occupational health service the provision of which is the responsibility
of the employer.
Eventually the creation of the Hungarian occupational
health service became connected to the so called programme for stabilisation.
In 1995 summer the No 89/1995 Governmental Order on Occupational Health
Services, signed by Lajos Bokros Minister of Finance, and the No 27/1995
Order of the Minister of Welfare on the Occupational health Services were
issued.
As for their contents the following are to be stressed.
The organisational structure of occupational health is in a state of transition.
Activity and structure of the services operate under the NPHMOS, professional
guidance is provided by the National Institute of Occupational Health.
The occupational health services may operate as:
Tasks of the primary service are:
The following measures were taken to solve the issues
above. At the end of 1995 the No 44/1995 WM order was issued to modify
the professional requirements determined by the No 27/1995 WM order. This
order solved the problem of missing physicians in the occupational health
services, though there was a big difference between the professional requirements
and the recommendations for specialisation.
In January, February, May and August 1996 further
assessments were made by NIOH, using a questionnaire and seeking answers
to the following questions:
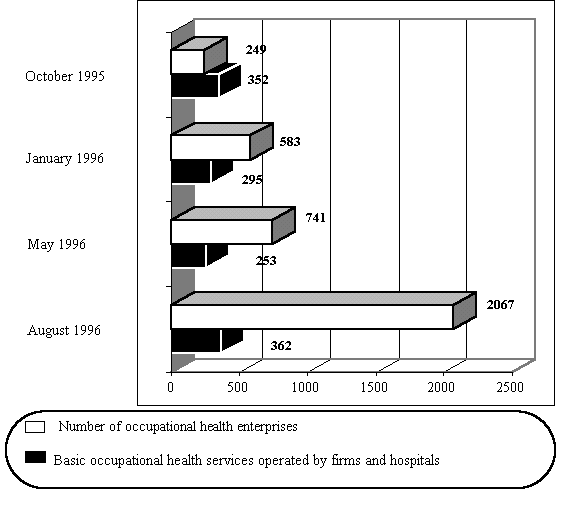 |
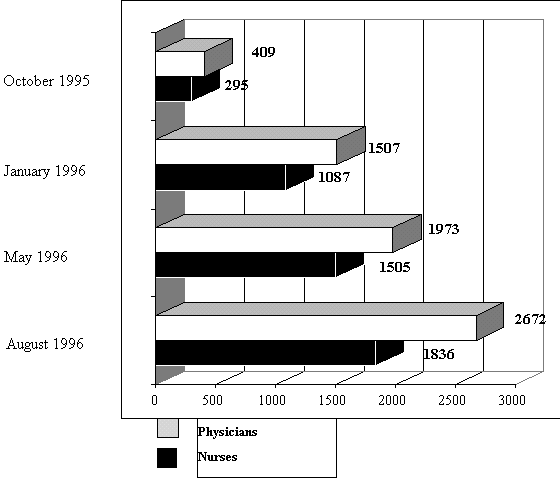
Figure 4. Number of occupational health physicians and nurses 1996 |
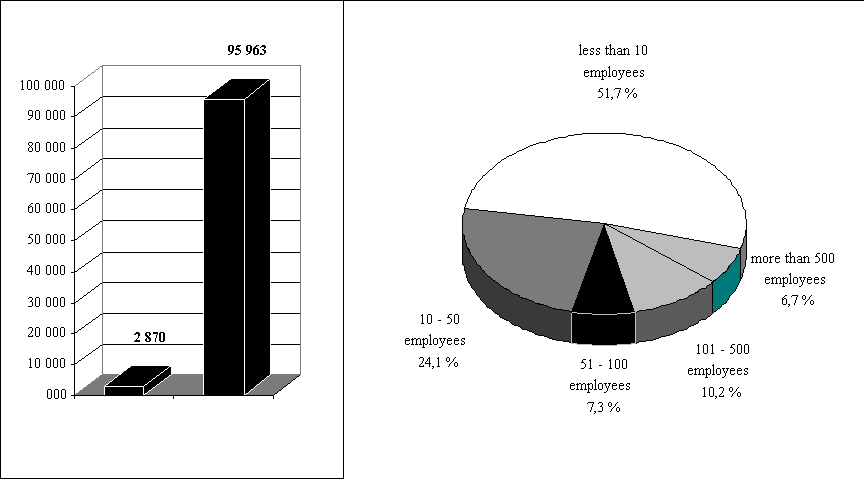
Figure 5. Number and size of enterprises with occupational health
service 1995
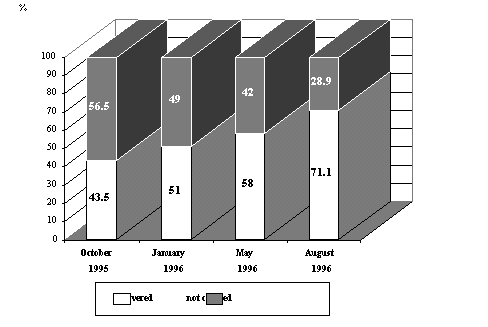
Figure 6. Percentage of employees covered by occupational health service between October 1995 and August 1996 |
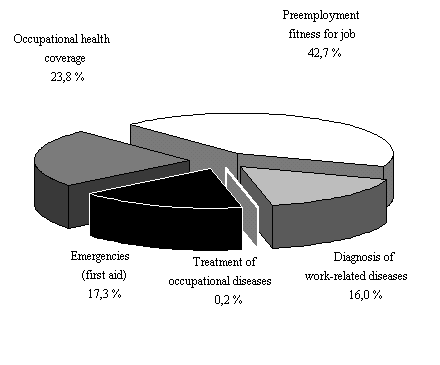
Figure 7. Occupational health activities within the consulting room in 1995 |
Figure 6 shows the changing percentage of the occupational health coverage of those working in organised employment. Two months after the transformation of the service 43.5 % of the employees were covered. In August 1996 this proportion was 71.1 % which proves the successful forming and development of the service. The most comprehensive provision exists in Finland, where coverage is more than 90 %. With the above mentioned result Hungary is among the first five countries in the world.
Transformation of the activity of the services also has been followed. Activities within and outside the consultation room were treated separately. The primary activities within the consulting room are the different types of fitness examinations (Fig. 7). Outside the consulting room activities are shown on Figure 8. The demonstrated data indicate that services do mainly preventive work, the number of occupational hygiene examinations and advising increased 10-fold, compared to the preceding years.
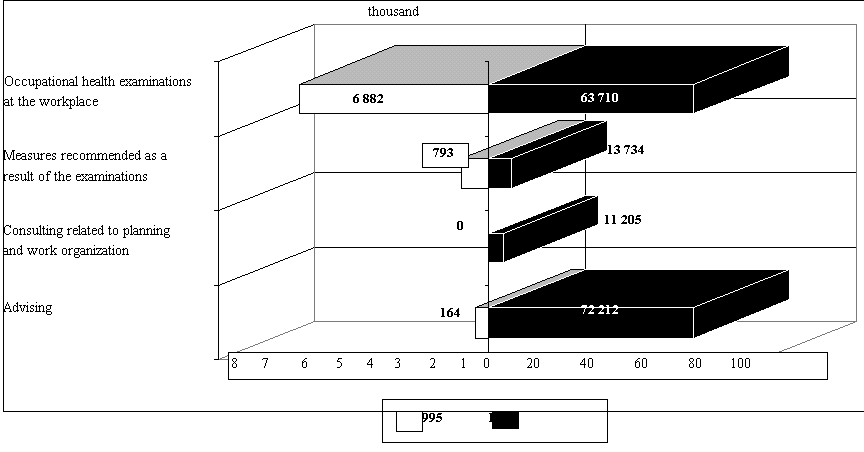
Figure 8. Occupational health activities outside the consulting
room in 1995 and 1996
Assessment data prove that successful privatisation, successful organisational and professional transformation have taken place in the field of occupational health. Regarding its organisation, tasks and operation a new type of service has emerged.
Transformation, of course, is a process that cannot be regarded as completed. While organisational transformation is relatively prompt, longer time is required for the transformation of attitude of the services, similarly to the achievement of adequate educational level and quality assurance. The next important steps of occupational health: organisation and operation of consultative services, education and training of specialist physicians and specialist nurses, updating of quality assessment and assurance systems.
NATIONAL AUTHORITY FOR WORK SAFETY AND LABOUR (OMMF) (1996). Information on the occurrence of work-related accidents (in Hungarian). Budapest.
NATIONAL INSTITUTE OF OCCUPATIONAL HEALTH (OMÜI) (1996). Occupational diseases and (intoxications) and excessive exposures. OMÜI, Budapest.
KAPRONCZAY K. (1988). Remarks on the development of the countrys industrial health until 1994 (in Hungarian). Ergonómia 198:211219.
UNGVÁRY GY. (1994). National Institute of Occupational Health: Occupational Health in Hungary. In: Publications of the National Institute of Occupational Health 19761990. NIOH Budapest pp.:1928.
UNGVÁRY GY. (1993). Occupational Health in Hungary. In: Occupational Health and National Development. (Yejaratnam, J., and Lim, S.C. eds). World Sci. Publ. Co. Pte Ltd River Edge. London, Hong-Kong, Banglore. 1993. Chapter 6. pp:120.
| Vol.3. No.1. |